Watch this short introduction to point of care ultrasound (POCUS), produced by the POCUS Journal team.
This article will provide a brief overview of what POCUS is, how these devices work, and the expanding clinical impact of their use.
A Classic Presentation
Imagine you are a family or emergency physician getting ready for a long shift. Maybe you practice in a rural area where advanced imaging is not readily available. Perhaps your clinic is backed up and quickly admit or send patients home. You first see a patient for shoulder pain with overhead activities. The next patient has abdominal pain in the right lower quadrant. The third has a tenderness on their leg after a recent flight. All of these conditions commonly require additional imaging for diagnosis. But, perhaps, there is a way to make a diagnosis immediately and expedite management.
What is Point of Care Ultrasound?
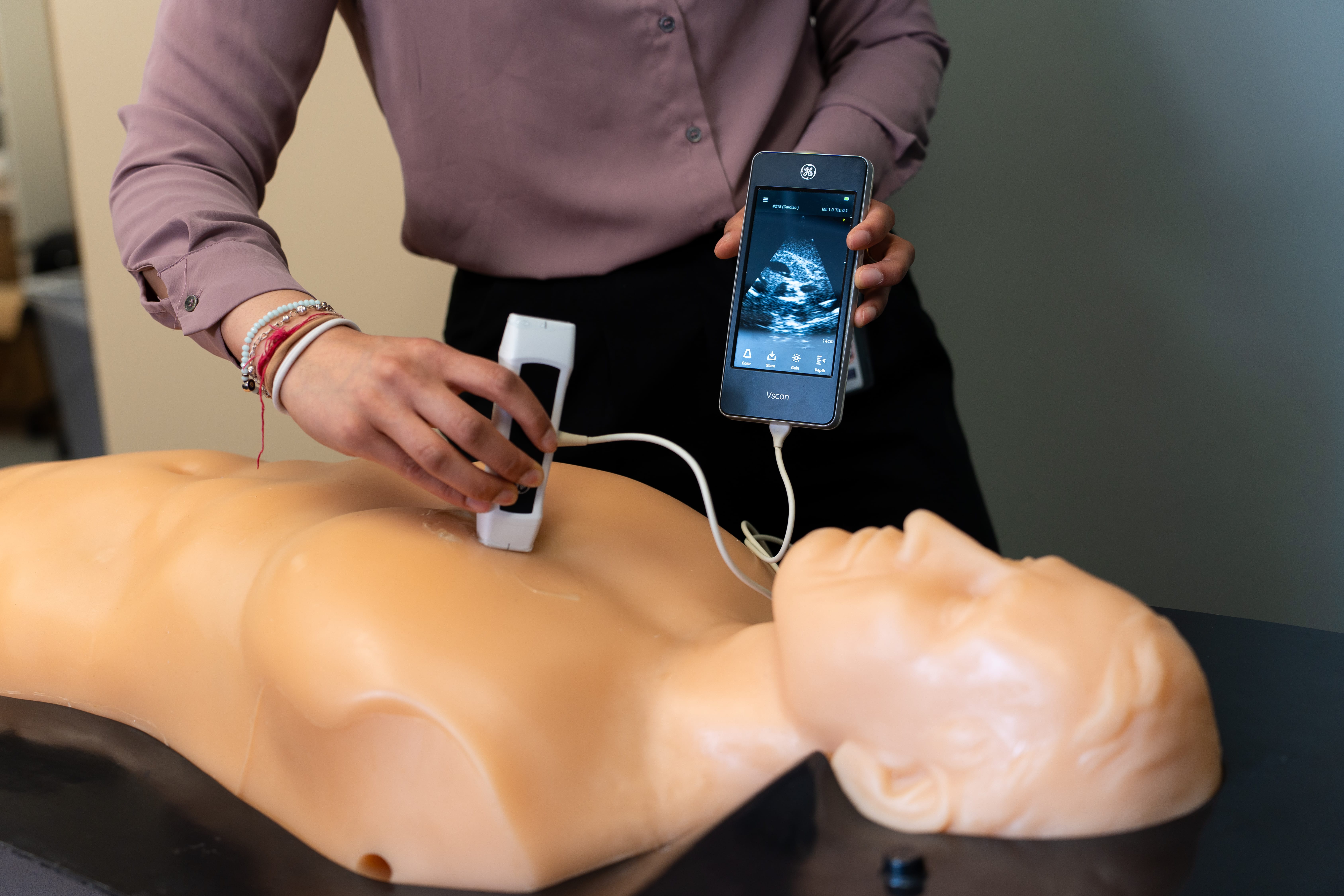
Point of care ultrasound (POCUS) describes the use of portable ultrasound systems at the bedside. These devices are commonly used by clinicians, nurses, and paramedics in hospitals, ambulances, and even in the remote wilderness. POCUS provides immediate diagnostic information to healthcare providers, enabling quick decisions on care. It complements traditional invasive/radiation-based imaging, supporting the choice of testing and reducing unnecessary scans.
What is the History of POCUS?
Ultrasound technology represents centuries of technological advancement, from the discovery of echolocation in bats, development of sonar in World War I, and eventual repurposing medical purposes in the 1940’s-1950’s.[1] The first use cases included identification of brain tumors by Dr. Karl Dussik, echocardiography by Dr. Inge Elder, and obstetrical use by Dr. Ian Donald. These first machines were large devices, requiring significant manual adjustment and time to produce grainy images.[1, 2] Patients were often required to submerge parts of the body in water in order for imaging to be successful.
Over time the technology improved. Ultrasound machines became smaller, allowing them to be placed on mobile carts. Ultrasound gel revolutionized the ease of acquiring images. In the 1990’s transducers became smaller and lighter. Battery technology started to improve. By the early 2000’s portable ultrasound devices no larger than a briefcase were in clinical across the world.
The 2010’s finally saw the emergency of modern-day POCUS. Small, pocket-sized devices that could be used like a stethoscope.
More about the history of POCUS
How Does POCUS Work?
POCUS devices rely on transducers, or probes, to generate predetermine frequencies of sound. Specialized materials in the probe and the ultrasound gel ensure that sound waves are efficiently transferred into the patient. Sound waves propagate through the tissue and reflect, refract, or scatter when coming in contact with air, fluids, tissues, or bone/calcium. These sound waves are returned to the device and translated to a visual image. This processing occurs almost instantaneously, allowing real-time decision making that directly influences patient care. Bluetooth-enabled devices can display images directly on a practitioner’s cellphone.

What Are Common POCUS Use Cases?
Novel information to guide the utility of POCUS or identify novel use cases are constantly being published in POCUS Journal. The following table lists some organ major systems and common conditions that can be assessed with POCUS.
| System | Example Conditions Diagnosable with POCUS |
| Cardiac | Pericardial effusion/tamponade, RV dilation, LV dysfunction |
| Respiratory | Pleural effusion, edema, atelectasis |
| Abdominal | AAA, bowel obstruction, stones, appendicitis |
| Musculoskeletal | Effusions, tendon tear (rotator cuff, Achilles) |
| Obstetrics | Ovarian cyst, confirm pregnancy location |
| Vascular | Deep vein thrombosis, perfusion |
| Trauma | FAST (free fluid), eFAST (pneumothorax), RUSH, ACES [3] |
What Are the Advantages of POCUS?
POCUS achieves immediate bedside answers, reducing time to diagnosis/treatment and decreasing the financial burden of advanced imaging. As a non-invasive and radiation-free imaging modality, it is safe to use on all patients at any stage of development. POCUS has been effectively applied to guide various bedside procedures including nerve blocks, intraosseous line placement, and IV line placement.[4, 5] It can be performed rapidly to assess resuscitation effectiveness over time in dynamic conditions such as sepsis.[6] The versatility of a handheld device has allowed POCUS to become an increasingly integral part of the physical exam in across disciplines and a wide range of practice settings, particularly those which are resource-limited.
What Are the Limitations of POCUS?
Like any emerging tool, POCUS requires education to be effective. Operator skill to manually move the probe, adjust parameters to acquire a clear image, and knowledge to interpret the image are critical. Imaging findings must always be interpreted with the clinical picture in mind.
Equally important is that practitioners recognize POCUS does not replace assessment with a dedicated cart-based ultrasound device. These machines offer a full range of imaging modes and probes. Under the guidance of an expert practitioner, they can achieve significantly higher resolution, deeper penetration, improved contrast, and reduced noise. Moreover, advanced imaging such as x-rays, CT scans, or MRIs are critical for high resolution assessment of patients. These gold-standard imaging tools should always be considered, especially if a POCUS scan is inconclusive or diagnosis is not certain. A lack of standardized guidelines can make it challenging to know when POCUS is most appropriate.

The Future of POCUS
Today, POCUS is being rapidly adopted in primary care and rural medical environments. Many physicians are seeking formal training for POCUS and identifying how these devices can be integrated into their practices. Many resources, such as POCUS Journal, are bridging the gap in resources needed for this education. With the ongoing efforts to integrate artificial intelligence into these devices to assist with interpretation, POCUS use will only get easier for novice practitioners.
Welcome to POCUS Journal
POCUS represents a change in the paradigm of how medicine is practiced at the bedside, improving the speed and accuracy of diagnoses.
We encourage our readers to explore additional articles, training materials, and resources across the POCUS Journal. With a continuous stream of impactful publications and posts, we are confident the time invested into engaging with this project will be fruitful on your learning journey with these devices.
References
- Rajamani, A., Arun Bharadwaj, P., Hariharan, S., Ragavan, A. V., Hassan, A., Arvind, H., & Huang, S. (2024). A historical timeline of the development and evolution of medical diagnostic ultrasonography. Journal of clinical ultrasound : JCU, 52(9), 1419–1437. https://doi.org/10.1002/jcu.23808
- What Is POCUS? A Brief History of Point of Care Ultrasound. (2023). GE Healthcare. https://www.gehealthcare.com/insights/article/what-is-pocus-a-brief-history-of-point-of-care-ultrasound
- POCUS: an introduction to point-of-care ultrasound technology. (2025). Philips. https://www.usa.philips.com/healthcare/article/pocus-introduction-point-of-care-ultrasound
- Bowling, J. M., & Zoumberakis, E. (2024). Ultrasound-Guided Nerve Blocks for Flexor Tenosynovitis. POCUS journal, 9(2), 12–14. https://doi.org/10.24908/pocus.v9i2.17395
- Plaut, I. S. Y., & Binder, Z. W. (2023). POCUS Confirmation of Intraosseous Line Placement: Visualization of Agitated Saline within the Right Heart in a Critically Ill Infant. POCUS journal, 8(1), 19–21. https://doi.org/10.24908/pocus.v8i1.16200
- Dalla Betta, M. B., Esener, D., Swanson, W., Kaddis, A., Aguayo Romero, F., & Fields, J. M. (2023). The Frequency of POCUS in the Treatment of Sepsis in the Emergency Department: A Retrospective Cohort Study. POCUS journal, 8(1), 71–80. https://doi.org/10.24908/pocus.v8i1.15683
Pingback: Let's Learn About POCUS #1: All About Transducers - POCUS Journal